Gallstone
| Gallstone | |
|---|---|
| Synonyms | Gallstone disease, cholelith, cholecystolithiasis (gallstones in the gallbladder), choledocholithiasis (gallstones in the common bile duct)[1] |
 | |
| Numerous small gallstones made up largely of cholesterol | |
| Pronunciation |
|
| Specialty | General surgery |
| Symptoms | None, crampy pain in the right upper abdomen[2][3][4] |
| Complications | Inflammation of the gallbladder, inflammation of the pancreas, liver inflammation[2][4] |
| Usual onset | After 40 years old[2] |
| Risk factors | Birth control pills, pregnancy, family history, obesity, diabetes, liver disease, rapid weight loss[2] |
| Diagnostic method | Based on symptoms, confirmed by ultrasound[2][4] |
| Prevention | Healthy weight, diet high in fiber, diet low in simple carbohydrates[2] |
| Treatment | Asymptomatic: none[2] Pain: surgery[2] |
| Prognosis | Good after surgery[2] |
| Frequency | 10–15% of adults (developed world)[4] |
A gallstone is a stone formed within the gallbladder out of bile components.[2] The term cholelithiasis may refer to the presence of gallstones or to the diseases caused by gallstones.[5] Most people with gallstones (about 80%) never have symptoms.[2][3] When a gallstone blocks the bile duct, a crampy pain in the right upper part of the abdomen, known as biliary colic (gallbladder attack) can result.[4] This happens in 1–4% of those with gallstones each year.[4] Complications of gallstones may include inflammation of the gallbladder (cholecystitis), inflammation of the pancreas (pancreatitis), jaundice, and infection of a bile duct (cholangitis).[4][6] Symptoms of these complications may include pain of more than five hours duration, fever, yellowish skin, vomiting, dark urine, and pale stools.[2]
Risk factors for gallstones include birth control pills, pregnancy, a family history of gallstones, obesity, diabetes, liver disease, or rapid weight loss.[2] The bile components that form gallstones include cholesterol, bile salts, and bilirubin.[2] Gallstones formed mainly from cholesterol are termed cholesterol stones, and those mainly from bilirubin are termed pigment stones.[2][3] Gallstones may be suspected based on symptoms.[4] Diagnosis is then typically confirmed by ultrasound.[2] Complications may be detected on blood tests.[2]
The risk of gallstones may be decreased by maintaining a healthy weight through sufficient exercise and eating a healthy diet.[2] If there are no symptoms, treatment is usually not needed.[2] In those who are having gallbladder attacks, surgery to remove the gallbladder is typically recommended.[2] This can be carried out either through several small incisions or through a single larger incision, usually under general anesthesia.[2] In rare cases when surgery is not possible medication may be used to try to dissolve the stones or lithotripsy to break down the stones.[7]
In developed countries, 10–15% of adults have gallstones.[4] Rates in many parts of Africa, however, are as low as 3%.[8] Gallbladder and biliary related diseases occurred in about 104 million people (1.6%) in 2013 and they resulted in 106,000 deaths.[9][10] Women more commonly have stones than men and they occur more commonly after the age of 40.[2]Certain ethnic groups have gallstones more often than others.[2] For example, 48% of Native Americans have gallstones.[2] Once the gallbladder is removed, outcomes are generally good.[2]
.mw-parser-output .toclimit-2 .toclevel-1 ul,.mw-parser-output .toclimit-3 .toclevel-2 ul,.mw-parser-output .toclimit-4 .toclevel-3 ul,.mw-parser-output .toclimit-5 .toclevel-4 ul,.mw-parser-output .toclimit-6 .toclevel-5 ul,.mw-parser-output .toclimit-7 .toclevel-6 ul{display:none}
Contents
1 Definitions
2 Signs and symptoms
2.1 Other complications
3 Risk factors
4 Pathophysiology
4.1 Composition
4.1.1 Cholesterol stones
4.1.2 Pigment stones
4.1.3 Mixed stones
5 Diagnosis
6 Prevention
7 Treatment
7.1 Surgical
7.2 Medical
8 Other animals
9 See also
10 References
11 External links
Definitions
Gallstone disease refers to the condition where gallstones are either in the gallbladder or common bile duct.[5] The presence of stones in the gallbladder is referred to as cholelithiasis, from the Greek chol- (bile) + lith- (stone) + -iasis (process).[1] If gallstones is in the common bile duct, the condition is referred to as choledocholithiasis, from the Greek chol- (bile) + docho- (duct) + lith- (stone) + iasis- (process).[1] Choledocholithiasis is frequently associated with obstruction of the bile ducts, which in turn can lead to cholangitis, from the Greek: chol- (bile) + ang- (vessel) + itis- (inflammation), a serious infection of the bile ducts. Gallstones within the ampulla of Vater can obstruct the exocrine system of the pancreas, which in turn can result in pancreatitis.
Signs and symptoms

Gallstones
Gallstones may be asymptomatic, even for years. These gallstones are called "silent stones" and do not require treatment.[11][12] The size and number of gallstones present does not appear to influence whether people are symptomatic or asymptomatic.[13] A characteristic symptom of gallstones is a gallstone attack, in which a person may experience colicky pain in the upper-right side of the abdomen, often accompanied by nausea and vomiting. The pain steadily increases for approximately 30 minutes to several hours. A person may also experience referred pain between the shoulder blades or below the right shoulder. Often, attacks occur after a particularly fatty meal and almost always happen at night, and after drinking.
In addition to pain, nausea, and vomiting, a person may experience a fever. If the stones block the duct and cause bilirubin to leak into the bloodstream and surrounding tissue, there may also be jaundice and itching. This can also lead to confusion. If this is the case, the liver enzymes are likely to be raised.[14]
Other complications
Rarely, gallstones in cases of severe inflammation may erode through the gallbladder into adherent bowel potentially causing an obstruction termed gallstone ileus.[15]
Other complications include ascending cholangitis if there is a bacterial infection which can cause purulent inflammation in the biliary tree and liver, and acute pancreatitis as blockage of the bile ducts can prevent active enzymes being secreted into the bowel, instead damaging the pancreas.[14] Rarely gallbladder cancer may occur as a complication.[6]
Risk factors
Gallstone risk increases for females (especially before menopause) and for people near or above 40 years;[16] the condition is more prevalent among both North and South Americans and among those of European descent than among other ethnicities. A lack of melatonin could significantly contribute to gallbladder stones, as melatonin inhibits cholesterol secretion from the gallbladder, enhances the conversion of cholesterol to bile, and is an antioxidant, which is able to reduce oxidative stress to the gallbladder.[17] Researchers believe that gallstones may be caused by a combination of factors, including inherited body chemistry, body weight, gallbladder motility (movement), and low calorie diet.[citation needed] The absence of such risk factors does not, however, preclude the formation of gallstones.
Nutritional factors that may increase risk of gallstones include constipation; eating fewer meals per day; low intake of the nutrients folate, magnesium, calcium, and vitamin C;[18] low fluid consumption;[19] and, at least for men, a high intake of carbohydrate, a high glycemic load, and high glycemic index diet.[20] Wine and whole-grained bread may decrease the risk of gallstones.[21]
Rapid weight loss increases risk of gallstones.[22] The weight loss drug orlistat is known to increase the risk of gallstones.[23]
Cholecystokinin deficiency caused by celiac disease increases risk of gallstone formation, especially when diagnosis of celiac disease is delayed.[24]
Pigment gallstones are most commonly seen in the developing world. Risk factors for pigment stones include hemolytic anemias (such as from sickle-cell disease and hereditary spherocytosis), cirrhosis, and biliary tract infections.[25] People with erythropoietic protoporphyria (EPP) are at increased risk to develop gallstones.[26][27] Additionally, prolonged use of proton pump inhibitors has been shown to decrease gallbladder function, potentially leading to gallstone formation.[28]
Cholesterol modifying medications can affect gallstone formation. Statins inhibit cholesterol synthesis and there is evidence that their use may decrease the risk of getting gallstones.[29][30]Fibrates increase cholesterol concentration in bile and their use has been associated with an increased risk of gallstones.[30]
Pathophysiology
Cholesterol gallstones develop when bile contains too much cholesterol and not enough bile salts. Besides a high concentration of cholesterol, two other factors are important in causing gallstones. The first is how often and how well the gallbladder contracts; incomplete and infrequent emptying of the gallbladder may cause the bile to become overconcentrated and contribute to gallstone formation. This can be caused by high resistance to the flow of bile out of the gallbladder due to the complicated internal geometry of the cystic duct.[31] The second factor is the presence of proteins in the liver and bile that either promote or inhibit cholesterol crystallization into gallstones. In addition, increased levels of the hormone estrogen, as a result of pregnancy or hormone therapy, or the use of combined (estrogen-containing) forms of hormonal contraception, may increase cholesterol levels in bile and also decrease gallbladder movement, resulting in gallstone formation.
Composition

From left to right: cholesterol stone, mixed stone, pigment stone.
The composition of gallstones is affected by age, diet and ethnicity.[32] On the basis of their composition, gallstones can be divided into the following types: cholesterol stones, pigment stones, and mixed stones.[3] An ideal classification system is yet to be defined.[33]
Cholesterol stones
Cholesterol stones vary from light yellow to dark green or brown or chalk white and are oval, usually solitary, between 2 and 3 cm long, each often having a tiny, dark, central spot. To be classified as such, they must be at least 80% cholesterol by weight (or 70%, according to the Japanese–classification system).[33] Between 35% and 90% of stones are cholesterol stones.[3]
Pigment stones
Bilirubin ("pigment", "black pigment") stones are small, dark (often appearing black), and usually numerous. They are composed primarily of bilirubin (insoluble bilirubin pigment polymer) and calcium (calcium phosphate) salts that are found in bile. They contain less than 20% of cholesterol (or 30%, according to the Japanese-classification system).[33] Between 2% and 30% of stones are bilirubin stones.[3]
Mixed stones
Mixed (brown pigment stones) typically contain 20–80% cholesterol (or 30–70%, according to the Japanese- classification system).[33] Other common constituents are calcium carbonate, palmitate phosphate, bilirubin and other bile pigments (calcium bilirubinate, calcium palmitate and calcium stearate). Because of their calcium content, they are often radiographically visible. They typically arise secondary to infection of the biliary tract which results in the release of β-glucuronidase (by injured hepatocytes and bacteria) which hydrolyzes bilirubin glucuronides and increases the amount of unconjugated bilirubin in bile. Between 4% and 20% of stones are mixed.[3]
Gallstones can vary in size and shape from as small as a grain of sand to as large as a golf ball.[34] The gallbladder may contain a single large stone or many smaller ones. Pseudoliths, sometimes referred to as sludge, are thick secretions that may be present within the gallbladder, either alone or in conjunction with fully formed gallstones.
Gallbladder opened to show small cholesterol gallstones

X-ray microtomograph of a gallstone

The large, yellow stone is largely cholesterol, while the green-to-brown stones are mostly composed of bile pigments
 Play media
Play media
CT images of gallstones
Large gallstone
Diagnosis
Diagnosis is typically confirmed by ultrasound. Other imaging techniques used are ERCP and MRCP. Gallstone complications may be detected on blood tests.[2]
A positive Murphy's sign is a common finding on physical examination during a gallbladder attack.
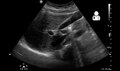
A 1.9 cm gallstone impacted in the neck of the gallbladder and leading to cholecystitis as seen on ultrasound. There is 4 mm gall bladder wall thickening.
Gallstones as seen on plain X-ray

Large gallstone as seen on CT
 Play media
Play media
A normal gallbladder on ultrasound with bowel peristalsis creating the false appearance of stones
Prevention
Maintaining a healthy weight by getting sufficient exercise and eating a healthy diet that is high in fiber may help prevent gallstone formation.[2]
The medication ursodeoxycholic acid (UDCA) appears to prevent formation of gallstones during weight loss.[35] A high fat diet during weight loss also appears to prevent gallstones.[35]
Treatment
Surgical
Cholecystectomy (gallbladder removal) has a 99% chance of eliminating the recurrence of cholelithiasis. The lack of a gallbladder may have no negative consequences in many people. However, there is a portion of the population—between 10 and 15%—who develop a condition called postcholecystectomy syndrome[36] which may cause gastrointestinal distress and persistent pain in the upper-right abdomen, as well as a 10% risk of developing chronic diarrhea.[37]
There are two surgical options for cholecystectomy:
- Open cholecystectomy is performed via an abdominal incision (laparotomy) below the lower right ribs. Recovery typically requires 3–5 days of hospitalization, with a return to normal diet a week after release and to normal activity several weeks after release.[11]
Laparoscopic cholecystectomy, introduced in the 1980s, is performed via three to four small puncture holes for a camera and instruments. Post-operative care typically includes a same-day release or a one night hospital stay, followed by a few days of home rest and pain medication.[11]
Medical
Cholesterol gallstones can sometimes be dissolved with ursodeoxycholic acid taken by mouth, but it may be necessary for the person to take this medication for years.[38] Gallstones may recur, however, once the drug is stopped. Obstruction of the common bile duct with gallstones can sometimes be relieved by endoscopic retrograde sphincterotomy (ERS) following endoscopic retrograde cholangiopancreatography (ERCP). Gallstones can be broken up using lithotripsy procedures, including laser lithotripsy and shock wave therapy.[38] These involve the breaking down of stones into tiny pieces that are then passed safely in the urine or feces.
Other animals
Gallstones can be a valued by-product of animals butchered for meat because of their use as a purported antipyretic and antidote in the folk remedies of some cultures, particularly, in China. The most highly prized gallstones tend to be sourced from old dairy cows, termed calculus bovis or niu-huang (yellow thing of cattle) in Chinese. Much as in the manner of diamond mines, some slaughterhouses carefully scrutinize workers for gallstone theft.[39]
See also
- Porcelain gallbladder
- Mirizzi's syndrome
References
^ abc Quick, Clive R. G.; Reed, Joanna B.; Harper, Simon J. F.; Saeb-Parsy, Kourosh; Deakin, Philip J. (2013). Essential Surgery E-Book: Problems, Diagnosis and Management: With STUDENT CONSULT Online Access. Elsevier Health Sciences. p. 281. ISBN 9780702054839..mw-parser-output cite.citation{font-style:inherit}.mw-parser-output .citation q{quotes:"""""""'""'"}.mw-parser-output .citation .cs1-lock-free a{background:url("//upload.wikimedia.org/wikipedia/commons/thumb/6/65/Lock-green.svg/9px-Lock-green.svg.png")no-repeat;background-position:right .1em center}.mw-parser-output .citation .cs1-lock-limited a,.mw-parser-output .citation .cs1-lock-registration a{background:url("//upload.wikimedia.org/wikipedia/commons/thumb/d/d6/Lock-gray-alt-2.svg/9px-Lock-gray-alt-2.svg.png")no-repeat;background-position:right .1em center}.mw-parser-output .citation .cs1-lock-subscription a{background:url("//upload.wikimedia.org/wikipedia/commons/thumb/a/aa/Lock-red-alt-2.svg/9px-Lock-red-alt-2.svg.png")no-repeat;background-position:right .1em center}.mw-parser-output .cs1-subscription,.mw-parser-output .cs1-registration{color:#555}.mw-parser-output .cs1-subscription span,.mw-parser-output .cs1-registration span{border-bottom:1px dotted;cursor:help}.mw-parser-output .cs1-ws-icon a{background:url("//upload.wikimedia.org/wikipedia/commons/thumb/4/4c/Wikisource-logo.svg/12px-Wikisource-logo.svg.png")no-repeat;background-position:right .1em center}.mw-parser-output code.cs1-code{color:inherit;background:inherit;border:inherit;padding:inherit}.mw-parser-output .cs1-hidden-error{display:none;font-size:100%}.mw-parser-output .cs1-visible-error{font-size:100%}.mw-parser-output .cs1-maint{display:none;color:#33aa33;margin-left:0.3em}.mw-parser-output .cs1-subscription,.mw-parser-output .cs1-registration,.mw-parser-output .cs1-format{font-size:95%}.mw-parser-output .cs1-kern-left,.mw-parser-output .cs1-kern-wl-left{padding-left:0.2em}.mw-parser-output .cs1-kern-right,.mw-parser-output .cs1-kern-wl-right{padding-right:0.2em}
^ abcdefghijklmnopqrstuvwxyzaa "Gallstones". NIDDK. November 2013. Archived from the original on 28 July 2016. Retrieved 27 July 2016.
^ abcdefg Lee, JY; Keane, MG; Pereira, S (June 2015). "Diagnosis and treatment of gallstone disease". The Practitioner. 259 (1783): 15–9, 2. PMID 26455113.
^ abcdefghi Ansaloni, L (2016). "2016 WSES guidelines on acute calculous cholecystitis". World journal of emergency surgery : WJES. 11: 25. doi:10.1186/s13017-016-0082-5. PMC 4908702. PMID 27307785.
^ ab Internal Clinical Guidelines Team (October 2014). "Gallstone Disease: Diagnosis and Management of Cholelithiasis, Cholecystitis and Choledocholithiasis. Clinical Guideline 188": 101. PMID 25473723.
^ ab "Complications". nhs.uk. Retrieved 13 May 2018.
^ "Treatment for Gallstones". National Institute of Diabetes and Digestive and Kidney Diseases. November 2017.
^ editors, Ronnie A. Rosenthal, Michael E. Zenilman, Mark R. Katlic, (2011). Principles and practice of geriatric surgery (2nd ed.). Berlin: Springer. p. 944. ISBN 9781441969996. Archived from the original on 2016-08-15.
^ Global Burden of Disease Study 2013, Collaborators (22 August 2015). "Global, regional, and national incidence, prevalence, and years lived with disability for 301 acute and chronic diseases and injuries in 188 countries, 1990-2013: a systematic analysis for the Global Burden of Disease Study 2013". Lancet. 386 (9995): 743–800. doi:10.1016/s0140-6736(15)60692-4. PMC 4561509. PMID 26063472.
^ GBD 2013 Mortality and Causes of Death, Collaborators (10 January 2015). "Global, regional, and national age-sex specific all-cause and cause-specific mortality for 240 causes of death, 1990-2013: a systematic analysis for the Global Burden of Disease Study 2013". Lancet. 385 (9963): 117–71. doi:10.1016/s0140-6736(14)61682-2. PMC 4340604. PMID 25530442.
^ abc National Institute of Diabetes and Digestive and Kidney Diseases (2007). "Gallstones" (PDF). Bethesda, Maryland: National Digestive Diseases Information Clearinghouse, National Institutes of Health, United States Department of Health and Human Services. Archived (PDF) from the original on 2010-12-05. Retrieved 2010-11-06.
^ Heuman DM, Mihas AA, Allen J (2010). "Cholelithiasis". Omaha, Nebraska: Medscape (WebMD). Archived from the original on 2010-11-20. Retrieved 2010-11-06.
^ Acalovschi, Monica; Blendea, Dan; Feier, Cristina; Letia, Alfred I.; Raitu, Nadia; Dumitrascu, Dan L.; Veres, Adina (2003). "Risk factors for symptomatic gallstones in patients with liver cirrhosis: a case-control study". The American Journal of Gastroenterology. 98 (8): 1856–1860. doi:10.1111/j.1572-0241.2003.07618.x. PMID 12907344.
^ ab "Gallstones (Cholelithiasis) Clinical Presentation: History, Physical Examination". emedicine.medscape.com. Archived from the original on 2016-11-14. Retrieved 2016-11-14.
^ Fitzgerald JE, Fitzgerald LA, Maxwell-Armstrong CA, Brooks AJ (2009). "Recurrent gallstone ileus: time to change our surgery?". Journal of Digestive Diseases. 10 (2): 149–151. doi:10.1111/j.1751-2980.2009.00378.x. PMID 19426399.
^ Roizen MF and Oz MC, Gut Feelings: Your Digestive System, pp. 175–206 in Roizen and Oz (2005)
^ Koppisetti, Sreedevi; Jenigiri, Bharat; Terron, M. Pilar; Tengattini, Sandra; Tamura, Hiroshi; Flores, Luis J.; Tan, Dun-Xian; Reiter, Russel J. (2008). "Reactive Oxygen Species and the Hypomotility of the Gall Bladder as Targets for the Treatment of Gallstones with Melatonin: A Review". Digestive Diseases and Sciences. 53 (10): 2592–603. doi:10.1007/s10620-007-0195-5. PMID 18338264.
^ Ortega RM, Fernández-Azuela M, Encinas-Sotillos A, Andrés P, López-Sobaler AM (1997). "Differences in diet and food habits between patients with gallstones and controls". Journal of the American College of Nutrition. 16 (1): 88–95. doi:10.1080/07315724.1997.10718655. PMID 9013440. Archived from the original on 2008-07-20. Retrieved 2010-11-06.
^ 4 Water | Dietary Reference Intakes for Water, Potassium, Sodium, Chloride, and Sulfate | The National Academies Press. p. 124. doi:10.17226/10925.
^ Tsai, C.-J.; Leitzmann, M. F.; Willett, W. C.; Giovannucci, E. L. (2005-06-01). "Dietary carbohydrates and glycaemic load and the incidence of symptomatic gall stone disease in men". Gut. 54 (6): 823–828. doi:10.1136/gut.2003.031435. ISSN 1468-3288. PMC 1774557. PMID 15888792.
^ Misciagna, Giovanni; Leoci, Claudio; Guerra, Vito; Chiloiro, Marisa; Elba, Silvana; Petruzzi, José; Mossa, Ascanio; Noviello, Maria R.; Coviello, Angelo; Minutolo, Marino Capece; Mangini, Vito; Messa, Caterina; Cavallini, Aldo; Michele, Giampiero De; Giorgio, Italo (1996). "Epidemiology of cholelithiasis in southern Italy. Part II". European Journal of Gastroenterology & Hepatology. 8 (6): 585–93. doi:10.1097/00042737-199606000-00017.
^ Choices, NHS. "Should you lose weight fast? - Live Well—NHS Choices". www.nhs.uk. Archived from the original on 2016-02-16. Retrieved 2016-02-16.
^ Commissioner, Office of the. "Safety Information—Xenical (orlistat) capsules". www.fda.gov. Archived from the original on 2016-06-11. Retrieved 2016-06-18.
^ Wang HH, Liu M, Li X, Portincasa P, Wang DQ (2017). "Impaired intestinal cholecystokinin secretion, a fascinating but overlooked link between celiac disease and cholesterol gallstone disease". Eur J Clin Invest (Review). doi:10.1111/eci.12734. PMID 28186337.
^ Trotman, Bruce W.; Bernstein, Seldon E.; Bove, Kevin E.; Wirt, Gary D. (1980). "Studies on the Pathogenesis of Pigment Gallstones in Hemolytic Anemia". Journal of Clinical Investigation. 65 (6): 1301–8. doi:10.1172/JCI109793. PMC 371467. PMID 7410545.
^ Endocrine and Metabolic Disorders: Cutaneous Porphyrias, pp. 63–220 in Beers, Porter and Jones (2006)
^ Thunell S (2008). "Endocrine and Metabolic Disorders: Cutaneous Porphyrias". Whitehouse Station, New Jersey: Merck Sharp & Dohme Corporation. Retrieved 2010-11-07.
^ M. A. Cahan, M. A.; L. Balduf; K. Colton; B. Palacioz; W. McCartney; T. M. Farrell (2006). "Proton pump inhibitors reduce gallbladder function". Surgical Endoscopy. 20 (9): 1364–1367. doi:10.1007/s00464-005-0247-x. PMID 16858534.
^ Kan, He-Ping; Guo, Wen-Bin; Tan, Yong-Fa; Zhou, Jie; Liu, Cun-Dong; Huang, Yu-Qi (2014-10-09). "Statin use and risk of gallstone disease: A meta-analysis". Hepatology Research. doi:10.1111/hepr.12433. ISSN 1386-6346. PMID 25297889.
^ ab Preiss, David; Tikkanen, Matti J.; Welsh, Paul; Ford, Ian; Lovato, Laura C.; Elam, Marshall B.; LaRosa, John C.; DeMicco, David A.; Colhoun, Helen M. (2012-08-22). "Lipid-modifying therapies and risk of pancreatitis: a meta-analysis". JAMA. 308 (8): 804–811. doi:10.1001/jama.2012.8439. ISSN 1538-3598. PMID 22910758.
^ Experimental investigation of the flow of bile in patient specific cystic duct models M Al-Atabi, SB Chin…, Journal of biomechanical engineering, 2010
^ Channa, Naseem A.; Khand, Fateh D.; Khand, Tayab U.; Leghari, Mhhammad H.; Memon, Allah N. (2007). "Analysis of human gallstones by Fourier Transform Infrared (FTIR)". Pakistan Journal of Medical Sciences. 23 (4): 546–50. ISSN 1682-024X. Archived from the original on 2011-08-24. Retrieved 2010-11-06.
^ abcd Kim IS, Myung SJ, Lee SS, Lee SK, Kim MH (2003). "Classification and nomenclature of gallstones revisited" (PDF). Yonsei Medical Journal. 44 (4): 561–70. ISSN 0513-5796. PMID 12950109. Retrieved 2010-11-06.
^ Gallstones—Cholelithiasis; Gallbladder attack; Biliary colic; Gallstone attack; Bile calculus; Biliary calculus Archived 2011-02-07 at the Wayback Machine. Last reviewed: July 6, 2009. Reviewed by: George F. Longstreth. Also reviewed by David Zieve
^ ab Stokes, Caroline S.; Gluud, Lise Lotte; Casper, Markus; Lammert, Frank (2014-07-01). "Ursodeoxycholic Acid and Diets Higher in Fat Prevent Gallbladder Stones During Weight Loss: A Meta-analysis of Randomized Controlled Trials". Clinical Gastroenterology and Hepatology. 12 (7): 1090–1100.e2. doi:10.1016/j.cgh.2013.11.031. ISSN 1542-3565.
^ Jensen (2010). "Postcholecystectomy syndrome". Omaha, Nebraska: Medscape (WebMD). Archived from the original on 2010-12-23. Retrieved 2011-01-20.
^ Marks, Janet; Shuster, Sam; Watson, A. J. (1966). "Small-bowel changes in dermatitis herpetiformis". The Lancet. 288 (7476): 1280–2. doi:10.1016/S0140-6736(66)91692-8. PMID 4163419.
^ ab National Health Service (2010). "Gallstones — Treatment". NHS Choices: Health A-Z—Conditions and treatments. London: National Health Service. Archived from the original on 2010-11-14. Retrieved 2010-11-06.
^ "Interview with Darren Wise. Transcrip". Omaha, Nebraska: Medscape (WebMD). Archived from the original on 2010-11-21. Retrieved 2010-11-06.
External links
| Classification | D
|
|---|---|
| External resources |
|
| Wikimedia Commons has media related to Gallstones. |
MedlinePlus Encyclopedia Gallbladder removal
- 5-Minute Clinical Consult Cholelithiasis
cholelithiasis US Classic gallstone with shadow and cholecystitis
Gallstones In-Depth Report from nytimes.com.







